 Does Medicare Cover Hospice?
Does Medicare Cover Hospice?
Many people are still not very familiar with Medicare and hospice. It is actually a fairly new idea. The “end of life movement” began in the ’70s. (The “end of life movement” is separate and distinct from the Euthanasia movement and organizations, like the Hemlock Society.) Medicare did not cover Hospice when Medicare started in 1965. Medicare and hospice were only put together in 1982 as part of the Tax, Equity, and Fiscal Responsibility Act under President Reagan in response to a growing awareness of end of life concerns. The legislation was an attempt to fill the gap in care. Awareness was growing in the country of the importance of what transpired at the end of life.
A Happy Death Is Not A New Idea
I remember when I was a teenager. My father was up before me in the mornings. He would take me to school on his way to work. I would see him praying when I came into the kitchen in the morning. One time I asked him what he was reading. It was a small devotional booklet. He was praying the novena to St. Joseph for a “Happy Death.” I was startled by the subject matter.
Teenagers don’t think much about death unless forced. I had a buddy, Herbert Woltz, killed in a motorcycle accident my senior year in high school. That was my abrupt intro to death.
I asked my father why pray for such a crazy thing as a “happy death”? The two subjects were oxymoronic to me. What’s happy about death? He reminded me that is how the Hail Mary ends. “Pray for us . . . now and at the hour of our death. Amen.”
After birth, he said, death is the most important event in your life. The difference, however, is you’re aware of what’s going on in the end, and you make the most important decisions of your life at “the hour of your death.” Praying for a “Happy Death” is about minimizing the pain and maximizing your moment of entrance into eternity. You’re asking for God and all the heavenly hosts to be at your side to handle the fear, pain, discouragement, and loneliness a person faces when approaching death and the moment of death.
I didn’t think much about what my father shared until many years had gone by and many friends and family members had passed away, including my dad. Medicare and hospice are something with which I have had extensive experience. Now I know why you would want to pay for a “happy death.”
End of Life Care Is Different
 As a seminary student in St. Paul, Minnesota in the early 80’s, I was looking for a part-time ministry when I wasn’t at school studying. I found the Hawthorne Dominicans. The Hawthorne Dominicans is a Catholic women’s religious order devoted to the terminally ill. They had a hospice facility near my college, so I would walk down to it and help out on weekends. Most of the patients were cancer patients. My work was minor cleaning, but mainly it was visiting with the patients. Keeping up their spirits. Show them someone cared as they were coming to the end of their lives, and I would join the sisters in prayer and mass for the residents.
As a seminary student in St. Paul, Minnesota in the early 80’s, I was looking for a part-time ministry when I wasn’t at school studying. I found the Hawthorne Dominicans. The Hawthorne Dominicans is a Catholic women’s religious order devoted to the terminally ill. They had a hospice facility near my college, so I would walk down to it and help out on weekends. Most of the patients were cancer patients. My work was minor cleaning, but mainly it was visiting with the patients. Keeping up their spirits. Show them someone cared as they were coming to the end of their lives, and I would join the sisters in prayer and mass for the residents.
While I was there, I got to know the sisters. They were remarkable young ladies. The convent was inside the hospice facility. The nuns lived, prayed, and worked with their dying residents around them twenty-four hours a day. The Hawthorne Dominicans were some of the happiest people I ever met.
Their foundress, Rose Lanthrop-Hawthorne, was the youngest daughter of the famous author, Nathanial Hawthorne, and a convert to Catholicism. In her day, cancer patients were put on an island in New York harbor–Blackwell Island–because it was believed that cancer was contagious. Many people, especially the poor, died in incredible misery, isolation, and squalor.
Medicare and hospice were a century away. Rose, like Mother Teresa of our time, saw the face of Jesus in the poor, and she started a ministry to the dying among the poor immigrants of the New York slums. The Hawthorne Dominicans is a purely American woman’s religious order. Most woman’s religious orders in our country came from Europe originally.
End of Life Care Rediscovered With Hospice & Medicare
The end of life movement in our time found its origin during a 1967 lecture at Yale University by Cicely Saunders. She introduced the idea that the dying needed specialized care that served their unique situation. She later founded St. Christopher’s Hospice in London.
Dr. Elisabeth Kubler-Ross, MD research into death and dying identified five stages terminally ill patients go through. Her popular and groundbreaking book, On Death & Dying, fueled a movement to deal with issues of death and dying.
In 1972 she testified at the first national hearings on death with dignity conducted by the U.S. Senator Special Committee on Aging. Organizations, like The National Hospice and Palliative Care Organization (NHPCO), sprang up to study and promote awareness around the end of life issues. Finally, because of raised public interest and concerns, Medicare added hospice care to the list of services provides in 1982.
Medicare And Hospice Are Huge
In 2014 approximately 2.6 million people died in the US. Of those deaths, 80% were on Medicare. Medicare is the largest insurer for persons during the last year of life. A quarter of the Medicare budget is just for those who are in the last year of life. That number has been consistent for decades. The high cost of health care at the end of life is not surprising considering the number and complexity of health issues, so CMS (Center for Medicare & Medicaid Services) is acutely aware of end of life issues.
life. A quarter of the Medicare budget is just for those who are in the last year of life. That number has been consistent for decades. The high cost of health care at the end of life is not surprising considering the number and complexity of health issues, so CMS (Center for Medicare & Medicaid Services) is acutely aware of end of life issues.
Today, hospice is an important benefit for terminally ill Medicare beneficiaries. Currently, nearly half of Medicare beneficiaries receive hospice benefits before their deaths. Medicare is the primary source of payment for hospice care in this country. Yet, hospice still remains somewhat of a mystery, and Medicare beneficiaries know very little about what Medicare does with hospice until they are forced into the situation.
How Does Medicare Cover Hospice?
Hospice is defined as a program of care and support for people who are terminally ill. Terminally ill means a life expectancy of six months or less. The primary goal of hospice in Medicare is to help terminally ill people live a comfortable life and manage their pain and discomfort. Hospice care is palliative care versus skilled nursing and home health care. That is, it is not designed to cure the patient, but rather to aid the person in the dying process. Because hospice care is so intimately involved and in such a big way with Medicare beneficiaries, understanding Medicare and hospice is essential.
Prayer to St. Joseph
O St. Joseph whose protection is so great, so strong, so prompt before the throne of God, I place in you all my interests and desires. O St. Joseph do assist me by your powerful intercession and obtain for me from your Divine Son all spiritual blessings through Jesus Christ, Our Lord; so that having engaged here below your heavenly power I may offer my thanksgiving and homage to the most loving of fathers. O St. Joseph, I never weary contemplating you and Jesus asleep in your arms. I dare not approach while He reposes near your heart. Press Him in my name and kiss His fine head for me, and ask Him to return the kiss when I draw my dying breath. St. Joseph, patron of departing souls, pray for us. Amen.
John Joseph Grimmond 1934-2013 R.I.P.
What Is Medicare Hospice?

Medicare pays for hospice, but what is hospice exactly?
Medicare defines hospice as a program of care and support for people who are terminally ill. Terminal illness, as Medicare definites it, is a life expectancy of six months or less. The primary goal of hospice in Medicare is to help terminally ill people live a comfortable life and manage their pain and discomfort. Hospice care is palliative care versus skilled nursing and home health care. Hospice does not cure the patient but rather aids the person in the dying process.
Death & dying is an area most people do not wish to ponder, so there are many misconceptions about Medicare-covered hospice care.
What Medicare Hospice Is Not?
Hospice is not a place. When my mother was terminally ill with ovarian cancer, I was thinking of taking her to a place.

When I was in college in the 80s, I had volunteered in a hospice facility run by the Hawthorne Dominican sisters. The hospice facility was an actual place people went to die. The nuns took care of everything: medical, personal care, food & lodging; and patients stayed there until the end.
That is what I had in mind when the doctors spoke to my family about hospice for our mother. That is not, however, how Medicare thinks of hospice.
Medicare does not pay for a hospice facility that provides room & board unless the care is tied to something like a skilled nursing facility. Medicare does, however, pay for hospice personnel and the medications they administer during hospice.
Where Do You Go For Hospice?
Hospice can be given virtually anywhere. A Medicare beneficiary can receive hospice at a hospital, hospice in a skilled nursing facility, hospice in an assisted living residence, and hospice at home. Medicare will pay for hospice care in assisted living, nursing homes, and other facilities if it is a Medicare-approved facility.
The end of life movement that started in the ’70s sees passing at home as the ideal. Most Medicare patients, when surveyed, prefer hospice in the home. That is where people feel most comfortable, but because of the level of care required, hospice care may have to move to a hospital in the last few days or another location.
Hospice can be given virtually anywhere.
Medicare.gov
What Kind of Illness Makes You Hospice Eligible?
When we think of hospice, we usually think of cancer, but there are other illnesses that result in hospice.
Grandpa Joe was 98. Grandpa had beaten cancer 4 times, lockjaw, and the Second World War. Dying didn’t seem possible. He had always been there, and we grandkids assumed he would always be there. Terminal illness and Grandpa Joe didn’t fit.
When Grandma Hilda announced to the family, Grandpa had congestive heart failure and was going into hospice, it didn’t quite register with us grandkids.
Grandpa Joe seemed the same old Grandpa Joe. When I was home from college, we chatted about the Cornhuskers, baseball, and politics. Nothing seemed to have changed, but there was a procession of nurses and therapists who came in and out of their home.
When Grandma Hilda finally called to tell us Grandpa had passed in his sleep, his death hit me like a sledgehammer.
Grandpa’s passing was hard on everyone, but Medicare providing and paying for hospice lightened the burden, especially for my parents and grandparents.

Who Can Go Into Hospice?
Hospice is also not exclusively for the old. I have a number of clients who are in their twenties and thirties. Not everyone on Medicare is sixty-five and older, though the majority are.
Accidents or illnesses permanently disabled some, and some are terminal. Hospice is for them too.
How Much Is Hospice?
Hospice care is not expensive for those on Medicare. Medicare pays for the vast majority of the hospice costs under Medicare Part A with very little out-of-pocket costs. Medications, some equipment, and nurses are covered.
Like I said earlier, hospice does not usually include custodial care or housekeeping. That can be very costly if the family cannot provide that type of care themselves.
How Do You Get Medicare To Pay For Hospice?
A Medicare beneficiary is eligible for Medicare’s hospice care benefit if she is entitled to Medicare Part A and meets the following conditions.
- The hospice doctor and the person’s regular physician certify that the person is terminally ill with a life expectancy of six months or less if the illness runs its
 expected course.
expected course. - The person accepts palliative care for comfort instead of care to cure her illness.
- The person must sign a statement choosing hospice care instead of other Medicare-covered treatments for her terminal illness and related conditions.
- The care is provided by a Medicare-certified hospice agency.
When these 4 critical are met, Medicare pays for hospice. At any time, a person may choose to exit hospice.
Is Hospice Euthanasia?
Hospice does not accelerate the dying process.
I have had people describe hospice to me as akin to euthanasia where someone actively terminates a life. Hospice is not euthanasia or assisted suicide. You do not intentionally cut short a person’s life. Hospice is about allowing the dying process to take its natural and inevitable course without assistance. Hospice care is about alleviating the suffering and providing comfort while the person dies.

An uncle of mine was a retired Omaha police captain. Uncle Bill had a severe stroke with many complications. He was put on a ventilator.
Uncle Bill was a strong and courageous individual. A vegetative existence was not for him not to mention impoverishing his wife with medical bills. He ordered the ventilator turned off.
Without the ventilator, he would quickly stop breathing. He knew it. The doctors made him as comfortable as possible with heavy sedation. His body fought hard against the loss of breath.
We gathered around his hospital bed. Over the course of a day, he passed peacefully from this life to next surrounded by his loving wife and children.
Hospice Is Up To You
I’ve known many individuals over the years who have gone on hospice for a time. Instead of dying, their health improved, or they resumed a normal life and quit hospice because the decline stopped. You are free to remove yourself from hospice at any time.
Hospice Is Also For The Living
Hospice is the option when all other alternatives have been exhausted. It is the option to bring the highest possible quality of life to a person’s remaining time. The hope is family members will look back on their time and know that everything was done to preserve, prolong, and then peacefully say goodbye.

While you may struggle with the challenge of terminal illness, the end of your life and hospice is as much about your loved ones as it is about you. Watching you suffer and your family’s grief afterward will be their burden. Dying is equally about them. Understanding that there is something for them as well as you in a scary time can give you all hope that the last great challenge in life will be a little less daunting.
While hospice ends with a patient’s death, family grief counseling can continue for up to a year. Medicare pays for that hospice care too.
One’s mortality is difficult to face, but the chance you will go on Medicare hospice at the end of your life is more than 50%. That is an extraordinary number, so having confidence Medicare will pay for hospice is critical.
 Why is Medicare Advantage Different When You Move?
Why is Medicare Advantage Different When You Move?
Medicare Advantage plans have lots of rules. When you move your permanent residence, those Medicare plan rules take effect.
As it states on the Medicare.gov website,
Medicare Advantage is another way to get your Medicare Part A and Part B coverage. Medicare Advantage Plans, sometimes called “Part C” or “MA Plans,” are offered by Medicare-approved private companies that must follow the rules set by Medicare. If you join a Medicare Advantage Plan, you’ll still have Medicare, but you’ll get most of your Part A and Part B coverage from your Medicare Advantage Plan, not Original Medicare.
These “bundled” plans include Medicare Part A (Hospital Insurance) Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. Medicare Part B (Health Insurance) covers doctors visits and outpatient procedures. Medicare Part D is for prescription drug coverage.
“Original Medicare” (Part A & Part B) is a Federal program. It is homogenous throughout the country. Original Medicare is the same in Maine as in Arizona.
Private insurance companies construct Medicare Advantage plans (MA plans) following Center for Medicare & Medicaid Services (CMS) regulations. They build the plans for a specific geographic location and are based upon a particular demographic population. CMS must approve all plans and continually monitors and audits those plans. Your Medicare Advantage changes when you move outside your current plan area.
build the plans for a specific geographic location and are based upon a particular demographic population. CMS must approve all plans and continually monitors and audits those plans. Your Medicare Advantage changes when you move outside your current plan area.
Medicare Advantage Is Local
Medicare Advantage plans are set up by county, a collection of conjoining counties, a state, or even regions, which can be multiple states. The insurance company needs a large enough pool of beneficiaries to scale the revenue, costs, and claims to design a plan that meets CMS’s (Center for Medicare & Medicaid Services) standards and is attractive to consumers. The number of plan participants in a geographic area determines a great deal about the plan. The geographic area of the plan is called the “service area.”
When a member of a particular plan leaves their “service area” permanently, they will no longer count as a member of that plan. In other words, your Medicare Advantage plan will change if you move. The member should contact their Medicare Advantage plan provider ahead of time. The member has several months to change to another plan with the same company in their new home area or to switch to a different insurance company that has a Medicare Advantage plan in their new location. Or, they can even return to Original Medicare and possibly purchase a Medicare Supplement.
Can I Use My Advantage Plan In Another State?
 You are covered anywhere within the U.S. in the case of an emergency. When traveling outside of your service area, your coverage depends upon the type of plan you have. You may be able to use your Medicare Advantage plan in another state, but you may not.
You are covered anywhere within the U.S. in the case of an emergency. When traveling outside of your service area, your coverage depends upon the type of plan you have. You may be able to use your Medicare Advantage plan in another state, but you may not.
An HMO (Health Maintenance Organization) plan generally includes only doctors and institutions in the network located in that service area. Some companies have “National Networks,” where an HMO member may tap into the national network for doctors and hospitals and pay in-network prices even though they are outside their service area.
The other type of plan is a PPO (Preferred Provider Organization) plan. You may access doctors in or out of the network. As long as the doctor or facility takes Medicare, you can get treatment from them. The out-of-network doctors and facilities will probably cost more than their in-network counterparts.
The Part D prescription drug part of the plan is less restrictive than the medical side. The network of pharmacies is more of the issue, but with a large number of national pharmacy chains with contracts with MA plans, you should be able to find your medications at approximately the same cost even away from home.
How Do I Switch My Medicare Advantage Plan If I Move?
Moving your Medicare Advantage plan to another state is very simple. Call the 800-number for customer service on the back of your MA medical card. Customer service at the insurance company will find you a comparable plan in your new location. Of course, they will only offer plans with their company.
comparable plan in your new location. Of course, they will only offer plans with their company.
You can also call your current agent. I receive phone calls every month from Medicare Advantage clients moving from one place to the next. Arizona and Florida seem to be the top choices currently. I can’t blame them! Texas and Colorado come in a distant second. I appreciate as much notice as you can give me so I can do some research before your move.
If you don’t have a relationship with a trusted insurance agent, you can certainly go on Medicare.gov and use their tool to find plans in the new area and do your own research when you move out of your Medicare Advantage plan service area.
The difficulty with the Medicare.gov “Find Plans” tool is the details of the plans are very general and incomplete. I use the Find Plans tool only for quick checks to see what insurance companies and plans are in the area. Then I go to my resources with the various insurance companies to do more in-depth research on the details of the plans.
 How Do I Find A New Medicare Advantage Plan?
How Do I Find A New Medicare Advantage Plan?
When a client calls me to let me know she’s moving to a new Medicare Advantage service area, I go to some aggregating tools that pull up the various Medicare Advantage plans for the new zip code.
I also check the Medicare Supplements in the new zip code as well in case the client wishes to move in that direction.
I also re-run their current medication list with dosages. Prescription drugs can be a significant determining factor between available policies, especially if the drugs are expensive.
Next, I compare their current plan to the future plans. Most of the time, people are moving their Medicare Advantage plan from the Omaha-Lincoln-Council Bluffs Metro area to an even higher population area, so the MA plans are often richer in benefits.
I help them sort through the plans weighing and sifting preferences and priorities until they settle on a plan that meets their needs. Then, depending on the time of the move, we execute the paperwork in person, via the internet, or snail mail. They receive their cards in approximately 10 days after approval and begin their new health coverage seamlessly. I follow up in a few months and during Annual Election Period (October 15th–December 7th) to make sure all is running smoothly.
What Are Some Problems For Medicare Advantage? 
As I said, most of my clients who move their Medicare Advantage plans are moving from eastern Nebraska and western Iowa to higher-population areas. The plans are quite often richer in other areas than here. The plans in Orange County, California, for example, are incredible! Many of the copays are zero and the dental, vision, hearing, and other extra benefits are huge in comparison to here.
Rural Areas
In almost a decade and thousands of clients, however, I had one couple move from here to Wyoming, into an area that was very rural even by Wyoming standards. There were NO MA plans in their new area at all. Those clients really wanted a Medicare Advantage plan.
Fortunately, it was their Initial Enrollment Period into Medicare for both of them, so we easily did a Medicare Supplement Plan N (coverage that fills in the gaps for the out-of-pocket expenses not covered by their Medicare Parts A and B) and Part D prescription drug plan instead.
As I said, that was a statistical anomaly, but it is a possibility. It is certainly something to consider when moving to a new Medicare Advantage service area, especially if you have health issues that may prevent you from passing Medicare supplement underwriting later on.
Can I Change My Medicare Advantage Plan if I Move?
 People quite often get fixated on “Medicare Open Enrollment,” which is from October 15th–December 7th every year. They think they are stuck and cannot change mid-year when they move. You can change your Medicare Advantage plan anytime when you move. You do not need to wait until the Annual Election Period (AEP) from October 15th–December 7th. You have what is called a Special Election Period (SEP) to adjust your Medicare plan.
People quite often get fixated on “Medicare Open Enrollment,” which is from October 15th–December 7th every year. They think they are stuck and cannot change mid-year when they move. You can change your Medicare Advantage plan anytime when you move. You do not need to wait until the Annual Election Period (AEP) from October 15th–December 7th. You have what is called a Special Election Period (SEP) to adjust your Medicare plan.
You need to notify your current Medicare Advantage plan of your move. You can also go through Medicare, or if you have a trusted agent licensed in the new state, you may be better served using them.
If you do not take care of your Medicare Advantage plan change when you move, there will be serious negative consequences for your health coverage, so do not delay!
The rule is you may make one change the month before your move, the month of your move, and up to two months after you move.
Moving is a difficult transition. I’ve done it too many times, in lots of different weather, to very distant and inconvenient places. Sometimes the move happens over a period of time. It is good to talk with someone who is knowledgeable about Medicare things to get help navigating the rules so you are not left out in the cold without health coverage.

Christopher Grimmond
Medicare is fantastic insurance. The MA plans have gotten stronger and stronger over the decade that I have offered them as well as more flexible and user-friendly. Medicare coverage will transfer easily to another state, but the rules are challenging. The best solution to all of these nuances is working with an insurance broker you trust. Omaha Insurance Solutions is ready to help you today! 402-614-3389.
 Finding a Medicare advisor in Omaha, NE, is not difficult. If you are turning 65, marketing companies sell your contact information, including birthday and phone numbers, to insurance agents. Lead companies are mailing you business reply cards (BRC) in hope that you will fill them out and mail them back in. Direct mail marketing companies are sending you postcards, flyers, and brochures because they want you to call their 800-Medicare number. Joe Namath and Jimmy J.J. Walker are on an endless loop of commercials coming into your living room telling you about the unbelievable Medicare benefits you do not qualify for. Dynomite!
Finding a Medicare advisor in Omaha, NE, is not difficult. If you are turning 65, marketing companies sell your contact information, including birthday and phone numbers, to insurance agents. Lead companies are mailing you business reply cards (BRC) in hope that you will fill them out and mail them back in. Direct mail marketing companies are sending you postcards, flyers, and brochures because they want you to call their 800-Medicare number. Joe Namath and Jimmy J.J. Walker are on an endless loop of commercials coming into your living room telling you about the unbelievable Medicare benefits you do not qualify for. Dynomite!
You will have to contact the FBI witness protection program to avoid the onslaught leveled against you as you approach Medicare eligibility!
Just Having An Insurance License Does Not Make You A Medicare Advisor
As you age into Medicare, an army is coming after you–an army of insurance agents. Some insurance agents, like me, have been around for a while. I earned my Nebraska & Iowa insurance licenses in 2003. Other agents just get their license for the Medicare Annual Election Period (AEP) when Medicare beneficiaries can change their Medicare plans. During those seven weeks of Medicare Annual Election Period AEP (Oct 15th–Dec 7th)–sometimes called “Open Enrollment”—Medicare insurance agents in Omaha, NE, are looking to make some money. They want to get new Medicare clients who are looking to change their Medicare plans.
earned my Nebraska & Iowa insurance licenses in 2003. Other agents just get their license for the Medicare Annual Election Period (AEP) when Medicare beneficiaries can change their Medicare plans. During those seven weeks of Medicare Annual Election Period AEP (Oct 15th–Dec 7th)–sometimes called “Open Enrollment”—Medicare insurance agents in Omaha, NE, are looking to make some money. They want to get new Medicare clients who are looking to change their Medicare plans.
People, however, are trying to find a Medicare advisor in Omaha, Ne, who is knowledgeable, competent, and trustworthy.
What Does It Take To Become A Medicare Insurance Agent in Nebraska?
 A Nebraska insurance license only means that you passed the licensing test and paid the $50 licensing fee. It doesn’t tell you how many times the person took the test to finally pass. It doesn’t tell you her score. You cannot even determine how long the person has been licensed, though you can find out their license number on the Nebraska Department of Insurance website.
A Nebraska insurance license only means that you passed the licensing test and paid the $50 licensing fee. It doesn’t tell you how many times the person took the test to finally pass. It doesn’t tell you her score. You cannot even determine how long the person has been licensed, though you can find out their license number on the Nebraska Department of Insurance website.
While doctors, lawyers, real estate agents, and even hairdressers go through a lengthy and difficult training and testing process, insurance agents for Medicare do not. I do not say this with any sort of pride, but as a matter of fact. Many of my fellow Medicare agents in Omaha, NE, have little or no training, are doing this as a temporary part-time gig, and/or will probably let their license drop at the end of the year.
Baby Boomers Increased The Demand For Medicare Advisors
Medicare health insurance is a federal program that began in 1965. The government created it because most insurance companies did not offer affordable health insurance to seniors. Congress intervened to create a program to protect seniors who were going bankrupt handling healthcare as the American population was living significantly longer in large numbers by the 1960s.
Insurance companies quickly developed insurance products to supplement Medicare where it was lacking. Insurance agents started selling these Medicare supplements. As the baby boomers started aging into Medicare, the demand exploded. There was more demand than what insurance companies and agencies could handle, so they began mass recruiting to find people to sell Medicare supplements. Recruiters promised the usual things to attract large numbers of people–huge sums of money and easy work.
supplements. As the baby boomers started aging into Medicare, the demand exploded. There was more demand than what insurance companies and agencies could handle, so they began mass recruiting to find people to sell Medicare supplements. Recruiters promised the usual things to attract large numbers of people–huge sums of money and easy work.
The sales pitch works because each year, thousands of people get their insurance licenses and become Medicare advisors in Omaha, NE, but quickly they find the work is not easy and they do not become rich overnight. Consequently, after they sell to a few friends and relatives, they let their license lapse. The people they signed up then lose their agent.
The Fallout from Poor Medicare Advisors
The consequence is Medicare beneficiaries are left on their own with an insurance product they probably do not understand in a health insurance program that is as foreign as a foreign language. The agent-less persons are now older. Their needs and circumstances are probably changed, and their income is even more limited. It is a bad situation.
While Medicare is not rocket science and I am not a brain surgeon, Medicare and Medicare insurance products have a certain level of complexity. A person needs a knowledgeable advisor to help them avoid pitfalls and maximize their benefits because Medicare and insurance products are always changing.
Independent Medicare Advisors in Omaha, NE
We are independent Medicare advisors in Omaha, NE. That means we do not work for an insurance company. We are not captive to an insurance company restricted to selling only one company or brand. We offer a large variety of companies in Nebraska and Iowa–the big names and the small. They all pay us the same commission, so there is no incentive to offer one company over the other. We are Omaha, Nebraska, Medicare insurance brokers, so we look for the best deal for our clients.
 How to Pick a Good Medicare Insurance Agent in Omaha, NE
How to Pick a Good Medicare Insurance Agent in Omaha, NE
First, we offer both Medicare Supplements and Medicare Advantage. These are both great options for those whom they fit. Our goal is to educate you on Medicare. The official Medicare handbook, Medicare & You, is over 120 pages of incredibly dull reading. We make it simple and understandable.
Secondly, we show you the actual Medigap and Medicare Advantage plans. Our software pulls together the policies and prices in nice neat rows and columns so you can compare and contrast. You can see the plans on one big four-foot computer screen, and we print out the quotes on one sheet of paper you can take with you.
From my experience, people come to us with separate quotes from various companies and a number of different agents. The mess of papers adds to your confusion. We pull the data up and let you see all the copays, co-insurance, maximum out-of-pocket, and premiums. It is only when you can look at them side-by-side on one computer screen and sheet of paper you can really see and compare.
We print out the quotes so you can take the material home with you. There shouldn’t be any pressure to decide or buy ‘right now.’ Picking a Medicare plan should not be a rush.
Finally, we find out about you and how you wish to manage your healthcare needs. Everyone is unique in how they wish to handle healthcare. Some of that has to do with your personality. Other reasons are your health. Your budget is an important determining factor. We work with you to see what fits you and is most comfortable for you.
Find A Medicare Advisor in Omaha, NE
You will be on Medicare hopefully for a long time. You want your Medicare advisor in Omaha, NE, to walk with you during that time to help you adjust and change as needs and times change. This is an important relationship for the long haul. Give us a call and find out how we help 402-614-3389.
When people talk about Medicare Part C or Medicare Advantage insurance plans in Omaha, Nebraska, they are usually making a comparison. The comparison is generally to Original Medicare and a Medicare Supplement with Part D. These are the two main ways most people get their Medicare. These two ways are very different, and I don’t believe it is really possible to make a legitimate comparison. But, as we used to say as kids, everyone does it. So let’s do it.
 Medicare Advantage Insurance Plans in Omaha Nebraska vs. Medigap
Medicare Advantage Insurance Plans in Omaha Nebraska vs. Medigap
The principal reason I don’t believe you can compare Medicare Supplements to Medicare Advantage is that Medicare Supplements are the same across the country. A Plan G in Arizona is the same as a Plan G in Maine. Medicare Advantage programs, however, are different from state to state and even from county to county. So I will compare Medicare Advantage insurance plans in Omaha, Nebraska, to Medicare Supplements here.
Low-Cost Medicare Advantage Plans in Nebraska
Price is the main attraction for many of my thousands of clients to Nebraska Medicare Advantage (MA plan). Most of the plans have no premium. A couple of them have minimal premiums, like $19, but the majority is zero. Clients like that, but they especially like the price in comparison to Medigap monthly premiums. A Plan G in this area for a male is approximately $150 per month on the low end. A drug plan could be $20 more or less. The simple math for a Plan G and a Part D prescription drug plan, including the Part B deductible, is around $2,200 a year. Most people do not spend anything close to that in annual copays on a MA plan.
Yes, one year or maybe two years, you might spend more than that on a Medicare Advantage plan in Nebraska, but over five, ten, fifteen years, most clients will pay out far less than the monthly Medigap premium that is constantly increasing with age and rate increases.
 Out of Control Medigap Premiums
Out of Control Medigap Premiums
Medicare beneficiaries constantly compare notes, which is an excellent source of referrals for me. I had a young lady come in recently. Her son, a client, brought her to the office to save money on her Medigap policy. She was 96 and paid $500+ per month for her Medicare Supplement. We submitted an application for a lower-cost Medigap policy since she was in good health. She passed, and we saved her over $3,000 a year. The cost of many Medigap policies can get entirely out of hand.
An agent should have been helping her keep her costs down all this time, but regardless, people see the price of supplements. They look at the Medicare Advantage insurance plan in Omaha, Nebraska, with no premium and very minimal copays, and they ask themselves, ‘Why?’
Why Pay Thousands of Dollars in Medigap Premium Each Year?
In the last analysis for most people, Medicare Advantage will result in less out-of-pocket costs than Original Medicare and a supplement and Part D plan in the long run. In the short run, most people will pay less with a Medicare Advantage plan. The general population recognizes this, which is why the continuous increase in enrollments throughout the country into Medicare Advantage plans.
 Medicare Advantage Insurance Plans in Omaha, Nebraska, Maximum Out-of-Pocket
Medicare Advantage Insurance Plans in Omaha, Nebraska, Maximum Out-of-Pocket
The downside of Medicare Advantage plans is when someone is seriously ill. One of my clients, a high school math teacher, developed leukemia, and the treatment was costly. The illness and treatment began in the fall. He hit his maximum out-of-pocket at that time, which was $4,900. The following year the treatments continued, and he reached the maximum out-of-pocket again. Dan was not happy about being on a Medicare Advantage plan. His cancer appeared a year after he started on the plan.
in the fall. He hit his maximum out-of-pocket at that time, which was $4,900. The following year the treatments continued, and he reached the maximum out-of-pocket again. Dan was not happy about being on a Medicare Advantage plan. His cancer appeared a year after he started on the plan.
We discussed switching to a supplement once his cancer went into remission. I waited two years and called Dan to do a supplement. Medigap plans usually have a two year gap required of being cancer-free. When we talked, he had decided to stay with the Medicare Advantage plan. He saw how over time, it saved him money. It must have been the math teacher in him. I was surprised, and I reminded him how upset he was a couple of years ago. He assured me that he was ok remaining on the plan, and he reminded me how emotional cancer can be.
I always remind people the maximum out of pocket is an actual number. The chances of one hitting that number at some point are real. I highly encourage clients to save the money they would otherwise spend on monthly premiums to offset the cost of copays and a challenging year.
Doctor Networks In Medicare Advantage Programs Omaha, Nebraska
Yesterday, I met with a lady who told me, “I don’t want a plan that tells me what doctors to see.” When I hear that phrase, I know they have listened to a Medicare Supplement advertisement or someone on YouTube deriding the evils of Medicare Advantage.
Medicare Advantage plans have networks just like the employer health plans most people were on most of their lives. Insurance companies develop networks for the purpose of keeping prices down.
As I said earlier, Medicare Advantage plans are local plans. They design the Medicare Advantage plan around a particular area, and the networks are no different. In the Omaha Metro area, which includes Lincoln, Bellevue, and Council Bluffs and all the small towns surrounding, there are three networks. Virtually every health professional in the area is associated with one or all of these networks. There are a couple of independent hospitals, but they also affiliate with the local Medicare Advantage plans in Omaha, Nebraska. In our area, there is absolutely no issue, and the networks and plans are going nowhere. These local plans and networks have been working together for years.
In other places, like Kansas City, where I have clients, the Medicare Advantage network criticism has some merit. I carefully check and double-check doctors and hospitals in that area because it is not as homogeneous as the Omaha Metro area. Of course, the Kansas City Metro is much more significant in terms of population and area. With 35 Medicare Advantage plans in Kansas Metro, finding the doctors and hospitals you prefer is not hard.
National Networks And PPO Plans
 But the network issue is actually becoming irrelevant as Medicare Advantage plans develop and grow. A larger and larger majority of doctors and medical facilities are becoming part of the MA network systems, and many of the insurance companies that offer Medicare Advantage plans also have national networks. With some plans, even HMO plans, clients may access doctors and hospitals across the country and pay in-network prices.
But the network issue is actually becoming irrelevant as Medicare Advantage plans develop and grow. A larger and larger majority of doctors and medical facilities are becoming part of the MA network systems, and many of the insurance companies that offer Medicare Advantage plans also have national networks. With some plans, even HMO plans, clients may access doctors and hospitals across the country and pay in-network prices.
For a while now, the insurance companies have included PPO (Preferred Provider Organization) plans. With a PPO plan, you have the in-network providers, like an HMO. Those doctors and medical facilities are at the lower in-network copays. The doctors and medical facilities not in-network cost a little more and have a higher total maximum out-of-pocket. As long as the doctor and hospital take Original Medicare, they will accept the PPO plan. Either way, this issue is becoming more and more a non-issue.
I also try to bring people back to reality. I ask, ‘How many times in your lifetime or your family have you left your area to go to a doctor or hospital over a hundred miles away?’ The reality for most people is zero. Sometimes the emotional sales language of the Medigap only insurance agents can cause a disconnect.
Managed Care
Medicare Advantage plans manage care like your employer’s health plans. The insurance company monitors the treatment you receive to make sure it is within customary standards of treatment. If not, the insurance company will question the requests. So the insurance company must approve a majority of the procedures before they are performed.
Original Medicare does not manage care in the same way. Providers must meet the same standard of care, but there is no thorough review or preapproval process.
Ironically in the same turn, Medicare hammers hard on the subject of Medicare fraud. CMS (Center For Medicare & Medicaid Services) encourages Medicare beneficiaries or whistle-blowers to report waste, fraud, and abuse, but they do not have the same preapproval process that would significantly reduce waste, fraud, and abuse.
 How To Stop Waste, Fraud, & Abuse?
How To Stop Waste, Fraud, & Abuse?
Fraud is fairly self-explanatory. It is financial gain through deception, but waste and abuse are what the insurance companies try to avoid through their managed care practices. Doctors will sometimes overprescribe. They recommend treatments that are more–and consequently more expensive–than is customary and necessary. For example, the doctor recommends an MRI for a shoulder problem instead of physical therapy to handle the issue. You might say to yourself that it’s up to the doctor, but there are customary and standard procedures of diagnosis and treatment. What would prevent a doctor from ordering a whole list of tests and procedures because he wants to be extra special careful.
An MRI is much more expensive than a couple of visits to the physical therapist that may solve the problem. If the physical therapist concludes that more than a few treatments are required to repair the issue or the treatment does not work, then the treatment moves to the next level, which may be getting an MRI at that point.
Some people may like that more liberal approach to health care. Original Medicare and Medigap policies will be a good fit. For those who are not concerned about the insurance company managing the care, as you experienced during your working years, then managed care or MA plans are a good fit.
Dental, Vision, Hearing, & More In Medicare Advantage Plans In Omaha, NE
 The feature that is a big attraction for Medicare Advantage plans is the additional benefits, such as dental, vision, fitness membership, etc. Original Medicare does not cover dental or vision in the form of eyeglasses. Those are benefits seniors want and do not want to pay an additional premium for a dental & vision plan.
The feature that is a big attraction for Medicare Advantage plans is the additional benefits, such as dental, vision, fitness membership, etc. Original Medicare does not cover dental or vision in the form of eyeglasses. Those are benefits seniors want and do not want to pay an additional premium for a dental & vision plan.
The Medicare Advantage insurance plans in Omaha, Nebraska have those benefits in varying amounts–teeth cleanings, $1,500 toward crowns & root canals, $300 for eyeglasses. The fitness memberships are attractive because it not only saves a member $500+ in gym fees annually, but it also gives them the flexibility to go to multiple gyms.
Part C or Medicare Advantage reduces the monthly cost for health coverage, provides broad access to doctors and hospitals, and adds additional benefits at little or no cost. For Medicare Advantage insurance plans in Omaha, Nebraska, the disadvantages that are problems in other places are not really issues here.
For those who do not wish to be on the hook for medical bills that may exceed $3,000 or $4,000 in a given year, MA plans may not be the best fit. If there is some concern that an insurance company may have more control over the management of their health care than Medicare itself, Original Medicare may be a better choice.
 So, What Questions Should You Ask Your Medicare Insurance Agent?
So, What Questions Should You Ask Your Medicare Insurance Agent?
What Is Medicare Advantage?
Sometimes there is confusion about Medicare Part C or Medicare Advantage insurance plans in Omaha, Nebraska. I have heard doctors’ offices call it “Medicare replacement plans” or “it is not Medicare.” So when asking what questions to ask your Medicare insurance agent, the definition of Medicare Advantage should be top of the list.
The key is in the name–Medicare Part C, like Medicare Part A and Part B. The Official Medicare.gov website says:”Medicare Advantage Plans are another way to get your Medicare Part A and Part B coverage. They are sometimes called “Part C” or “MA Plans,” which are offered by Medicare-approved private companies that must follow the rules set by Medicare.”
Medicare mandates what the private insurance companies cover and even how they cover patients’ needs. The monitoring is incredible. This is definitely a question you should ask your Medicare insurance agent.
When I moved into my neighborhood, I got to know my next-door neighbor. He was a partner in a large public accounting firm in Omaha. When he saw my license plate–it says “Medigap”–he asked me to guess who his most prominent client was.
CMS (Center for Medicare and Medicare Services) administers Medicare. CMS is an enormous bureaucracy, but they do not have the capability to monitor something as complex and large as many insurance companies, so they hire auditors. My neighbor’s biggest client is Medicare.
His firm and many other accounting firms audit the financial and billing records of the insurance companies offering Medicare Advantage because Medicare is not directly administering the insurance programs like they administer Medicare Part A and Part B. Small world.
Even though private insurance companies design and administer the Medicare Advantage plans. “Medicare Advantage Plans must cover all of the services that Original Medicare covers,” as it says on Medicare.gov. Confused? These are questions you should ask your Medicare Insurance agent.
What Other Questions Should You Ask Your Medicare Insurance Agent?
Why Medicare Advantage?
In the early 1970s, Congress was trying to figure out how to keep the costs down for Medicare. They imagined involving private insurance companies and creating an atmosphere of competition. Over the decades, the program developed into what is now Medicare Part C or Medicare Advantage.
The number of Medicare beneficiaries on Medicare Advantage is over 40% and growing each year as the plan strengthens. The plans improve health outcomes from beneficiaries, more benefits, and lower costs to Medicare.
How Does Medicare Advantage Work?
How Medicare Advantage works is a question that you should ask your Medicare insurance agent. CMS, in effect, hired a private insurance company to develop a Medicare plan. The plan gives the same coverage as Medicare Part A and Part B. CMS pays the insurance companies an amount based upon the number of clients, ages, services, and outcomes. The formulas to determine payment have become increasingly complex as CMS and the insurance companies try to devise a system that motivates healthcare workers, institutions, and insurance companies to curtail costs and improve health outcomes.
 You Should Ask Your Medicare Insurance Agent How To Compare Medicare Advantage To Medigap
You Should Ask Your Medicare Insurance Agent How To Compare Medicare Advantage To Medigap
Each type of Medicare plan is structured the same from place to place. The plans, however, vary in costs. High population centers like cities will have very rich plans compared to isolated rural areas.
They are not like Medigap plans that work with Medicare Part A and Part B, which are universally the same from one part of the US to the next. The population has absolutely no effect on Part A and Part B. The Medigap plans maybe even less in rural areas because older populations tend to move to higher population areas around doctors and hospitals. Thus Medigap claims in rural areas are fewer and smaller.
You cannot compare Medicare Advantage to Medigap in any way that is fair. They have two separate and distinct delivery systems for health care. Those who do attempt comparisons are usually building straw men to know down to serve their purposes.
One of the Most Important Questions to Ask Your Medicare Insurance Agent:
What To Look For In A Medicare Advantage Plan?
The first metric I like to consider is the maximum out-of-pocket. The maximum out-of-pocket (MOOP) is how much you potentially could spend out of your pocket while on that particular health plan in one year. During your working years, your employer’s health plan had a MOOP.
Many people confuse MOOP with a deductible. A deductible is the amount of money you pay before the plan begins to cover medical costs. For example, you have a $2,000 deductible. You go to the emergency room, and the bill is $20,000. You pay the first $2,000 upfront.
Then, you pay a coinsurance of 20% on the next $18,000, which would be $3,600 ($18,000 x 20% = $3,600).
This is how the maximum out-of-pocket (MOOP) works. The $2,000 deductible + $3,600 coinsurance = $5,600. If the MOOP is $6,000, you would pay $5,600. If the MOOP was $5,000, you would pay $5,000. This information is crucial, and it should definitely be part of the questions that you ask of your Medicare insurance agent.
 Maximum Risk
Maximum Risk
I see the maximum out-of-pocket as the most important number because that is your potential maximum risk, which is why it’s so important to ask questions of your Medicare insurance agent about it. While it is highly unlikely that you will arrive at the maximum each year or any given year, there is some probability. Because of that chance, you should be prepared to cover that expense because you are contractually obliged.
If you have two years back-to-back of expense–imagine chemo and radiation for cancer over a year’s time–you could conceivably have two consecutive years together when you reach your MOOP both years. While the probability of hitting that maximum is very low, the possibility is always there.
You can either cover that risk by purchasing a Medigap policy instead of a Medicare Advantage plan and pay the monthly premium or save that amount each month until you have reserves equal to or greater than your MOOP.
When looking at Medicare Advantage plans in Omaha, Nebraska, the first number I look at is your maximum risk–the maximum out-of-pocket (MOOP).
What Other Questions Should You Ask Your Medicare Insurance Agent?
Medicare Part C Many Times Include Prescription Drug Coverage
Most Medicare Advantage also includes the Part D prescription drug plan, especially Medicare Advantage Plans in Omaha, Nebraska. I would run your medications through the Medicare.gov plan finder before going any further in plan selection. Many times I thought I had the best plan picked out, and then I come to find certain medications for that person or not covered. Or the cost of the medications is significantly higher than on other plans. Check the medications before doing anything else.
While you can ask for drug exceptions from a plan, I would absolutely not go into a new plan with that expectation. Ask your Medicare insurance agent to make sure all of the medications are covered and covered at a reasonable rate compared to the other plans in the area.
 They Tell You What Doctor to Go See
They Tell You What Doctor to Go See
Many times I will hear someone say, ‘Medicare Advantage plans tell you what doctors to see.’ When I hear that, I know that person only sells Medigap policies. Here’s a prime example of when you need a Medicare insurance agent to ask questions from.
Networks are important. The Medicare Advantage insurance plans in Omaha Nebraska are embedded in the three hospital network systems here.
You, of course, want to go to the medical professionals with whom you already have relationships. All three networks work with the principal insurance companies offering Medicare Advantage in the area. Those doctors, hospitals, and clinics are in-network. Even the few independent firms in the area also have relationships with the plans.
In other areas, the plans may not be as connected. You need to verify your doctors and hospitals before considering a plan.
What Are The Copays?
A question you need to ask your Medicare insurance agent is: what are the copays? Once you have determined the amount of MOOP you are comfortable assuming, verified your prescriptions and doctors, you look at the copays. Everyone has their own way of evaluating prices. Compare the various copays among plans, doctors, x-rays, MRI’s etc. Narrow down the number of plans. There is no perfect plan. There are always trade-offs.
Extra Benefits in Medicare Advantage Insurance Plans in Omaha, Nebraska
Many people focus on the extra benefits that Medicare Advantage offers, like dental and vision. Those are real benefits and should be weighed. However, dental expenses are usually not life-threatening nor do they run into the tens of thousands like health insurance or prescription drugs. This is a crucial place to ask questions of your Medicare insurance agent.
A particular plan may have a nice dental benefit of $1,500, but if the MOOP on that plan is $7,000 versus another plan with no dental at a $2,800 MOOP, I would favor the plan with the small MOOP. You can always purchase a separate standalone dental plan.
No Underwriting
Many people do not realize that Medicare Advantage plans do not have underwriting like Medigap plans. During your Annual Election Period (AEP) October 15th–December 7th, you may change from one plan to the other without answering any health questions. The plan cannot refuse you. You may also change during the course of the year if you have a special reason for changing.
You Can Change During Annual Election Period (AEP) October 15th-December 7th
The Annual Election Period is the time when you may change your Medicare Advantage Plan. You don’t need a reason, but you could have one. You are not happy with the service. Another plan appears with richer benefits or lower MOOP and copays. You plan on doing extensive dental work and you want a plan with more dental for that year. There can be multiple reasons or no reasons for changing. You may change.
 Ask Your Medicare Insurance Agent: Does Your Plan Have A National Network?
Ask Your Medicare Insurance Agent: Does Your Plan Have A National Network?
A concern people have with Medicare Advantage plans is with the network. The network concerns extend quite often beyond the local area. People are concerned about travel, outside of the service area, going to specialists not located in the service area.
Many of the major insurance carriers, including in the Omaha Metro area, have national networks. That is, you can go to doctors and hospitals outside of the local service area and still be in-network and pay in-network prices because the doctors and hospitals participate in the insurance company’s national network. This includes HMO (Health Maintenance Organization) plans. PPO (Preferred Provider Organizations) plans cover doctors and hospitals by design out of the local area. You may pay more, but you will have access. For emergencies, you are covered anywhere on Medicare Advantage plans. For some people, especially those who may travel, this is a concern.
Medicare is incredible health insurance. It comes in various forms to fit your needs and how you wish to be serviced. Medicare Advantage Insurance Plans in Omaha, Nebraska are a powerful way to receive your Medicare. Understanding the trust about Medicare Advantage and sorting through the exaggerations and distortions is important to make sure your needs are authentically served.
 Medicare Advantage and Home Health Care
Medicare Advantage and Home Health Care
All Medicare Advantage (MA) plans must provide at least the same level of coverage for home health care as does Original Medicare, so Medicare Advantage pays for home health care. However, an MA plan may have different rules, costs, and restrictions on services. For example, depending on a person’s MA plan, it may require him to:
- Obtain care from a home health agency that has contracted with the plan.
- Receive prior authorization or a referral before receiving home health care.
- Pay a copayment for home health care.
Coverage of Non-Skilled Care and Other In-Home Support Services
Center for Medicare & Medicaid Services (CMS) recently announced that Medicare Advantage plan will be able to cover certain types of home health care related services that were not previously able to be offered, beginning in 2019. This will be possible because CMS has expanded the definitional scope of “supplemental benefits” that Medicare Advantage plans can offer. Starting in 2019, insurers can offer additional services to help improve enrollees’ health and quality of life.
Medicare Advantage Can Pay for Home Health Care Supplemental Benefits
Medicare Advantage plans may offer additions benefits not offered by Original Medicare. Previously, CMS did not allow any item or service to qualify as a supplemental benefit. Supplemental benefits were items of “daily maintenance.” In other words, MA plans could not offer items and services that were not directly for medical treatments. The agency has now reinterpreted the requirement for supplemental benefits to include a “primarily health-related” definition as follows:
an item or service that is used to diagnose, prevent, or treat an illness or injury, compensate for physical impairments, act to ameliorate the functional/psychological impact of injuries or health conditions, or reduce avoidable emergency and healthcare utilization
Some Medicare Advantage Supplemental Benefits
Accordingly, this reinterpretation of supplemental benefits will allow Medicare health plans to offer coverage or benefits for the following:
- Adult daycare services are services provided outside the home, such as assistance with activities of daily living (ADLs) and instrumental activities of daily living (IADLs)
- In-home support services are services a personal care attendant provides. She assists disabled or medically needy individuals with activities of daily living, such as eating, bathing, and transferring, and instrumental activities of daily living. These activities may include managing money, preparing meals, and cleaning a house. Services must be performed by individuals licensed to provide personal care services, or in a manner that is otherwise consistent with state requirements.
- Home-based palliative care services Medicare does not cover if life expectancy is more than six months. Palliative care (“comfort care”) is to diminish symptoms of a terminally ill patient.
- Transportation for nonemergency medical services is transportation to obtain Part A, Part B, Part D, and supplemental benefit items and services. The
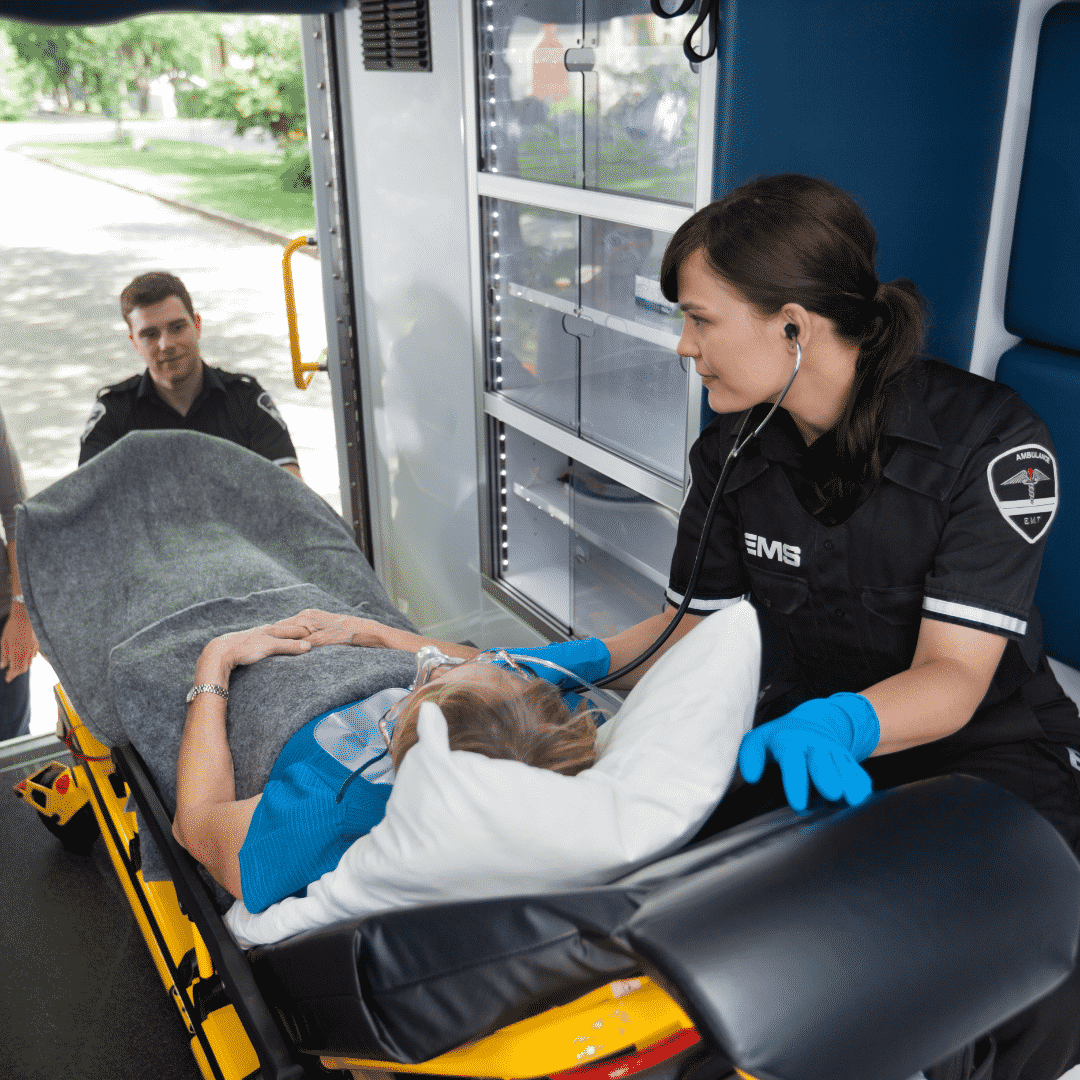 transportation must be used to accommodate the enrollee’s health care needs: it cannot be used for nonmedical services, such as groceries or errands.
transportation must be used to accommodate the enrollee’s health care needs: it cannot be used for nonmedical services, such as groceries or errands. - Home safety devices and modifications are safety devices to prevent injuries in the home and/or bathroom. The modifications must be non-structural and non-Medicare covered. This benefit can include home and/or bathroom safety inspection to identify any need for safety devices or modifications.
A physician or licensed medical professional must recommend these home care services.
Medicare’s expansion of MA plan benefits, like adult days care, helps patients remain in their homes as they age rather than being institutionalized, which could also result in lower costs for Medicare and Medicaid.
 The Advantage of Medicare Advantage for Home Health Care
The Advantage of Medicare Advantage for Home Health Care
Medicare Advantage plans may impose different rules, limitations, and costs than Original Medicare, but they must provide at least the same level of home health care benefits.
Starting in 2019, Medicare Advantage plans may offer supplemental benefits that help enrollees with daily maintenance, including transportation for medicare services, in-home support services, and home-based palliative care. Consult the individual MA plan for the details of coverage.
In the Omaha metro area, the MA plans offer some of these benefits. Currently, the plans that do offer a lot of these benefits are the “Dual” or “Special Needs” plans. Those plans are for a person on full Medicaid as well as Medicare or have some special needs because of chronic illness, such as COPD, Diabetes, etc.
In other areas with high population densities, many of the MA plans are much richer with benefits. As it stands in eastern Nebraska and western Iowa, principally Omaha, Lincoln, Bellevue, and Council Bluffs, the supplemental benefits seem to be growing in number and scope each year. A couple of insurance companies recently added transportation to their health plans. More insurance companies are developing Medicare Advantage plans and including this type of home health services.
 Navigating the Complexities: What You Need to Know About Medicare and Home Healthcare Coverage
Navigating the Complexities: What You Need to Know About Medicare and Home Healthcare Coverage
Are you confused about Medicare and home health care coverage? If so, you’re not alone. Navigating the complexities of these topics can be overwhelming. It’s essential to understand your options and ensure you receive the care you need.
Does Medicare pay for home health care services?
This article will delve into the ins and outs of Medicare and home healthcare coverage, providing the information you need to make informed decisions. We’ll explore the different types of Medicare plans and how they relate to home healthcare services, eligibility requirements, coverage limitations, and common misconceptions.
Whether you’re a senior seeking assistance or a caregiver supporting a loved one, understanding how long Medicare pays for home health care is crucial. By the end of this article, you’ll clearly understand what options are available and how to navigate the complex healthcare landscape.
Stay tuned to discover everything you need about Medicare and home healthcare coverage. Don’t let the confusion hold you back from accessing the care you deserve.
Different Types of Medicare Coverage
Medicare is a federal health insurance program that covers people over 65 and those with specific disabilities or chronic conditions. There are several types of Medicare plans, each with benefits and limitations. Knowing how long each Medicare plan pays for health care is critical. 
Original Medicare, also known as Medicare Part A and Part B, provides coverage for hospital stays, doctor visits, home healthcare, and some medical equipment. Medicare Part C, also known as Medicare Advantage, is a private insurance option combining Parts A and B, often including additional benefits such as prescription drug coverage and dental care. Both provide home healthcare coverage, but in specific ways unique to the plans.
Medicare Part D provides coverage for prescription drugs, while Medicare Supplement plans, also known as Medigap, help cover the costs of out-of-pocket expenses not covered by Original Medicare.
Understanding the differences between these plans is essential because they approach home health care differently.
 Understanding Home Healthcare Services
Understanding Home Healthcare Services
As the name suggests, home healthcare services provide medical care and support to individuals in their homes. This can include services such as nursing care, physical therapy, and speech-language therapy. Home health care is often a more convenient and cost-effective option than hospital or skilled nursing facility (SNF) care and can provide a higher level of comfort and independence for patients. It is skilled nursing care but provided in the home for those who would not have access to medical care otherwise.
The purpose of home health care is short-term treatment for an illness or injury, such as a stroke or broken hip. It is about getting back your health and independence again.
For the chronically ill and disabled, the goal of home health care is to maintain the highest level of ability and health.
Home healthcare services can be provided by a variety of healthcare professionals, including registered nurses, licensed practical nurses, physical therapists, occupational therapists, and speech-language pathologists. A physician typically orders services, and they are covered by Medicare and/or private insurance.
Home health care is not home care. Home care would be custodial services like housekeeping, bathing, feeding, etc. Medicare does not usually provide those types of personal services, strictly speaking. There are exceptions, however. On occasion, Medicare allows for a temporary home health aide to assist in the healing process.
Some injuries and illnesses may last for a long time. While home health care is a necessary service, the bigger question is: how long does Medicare pay for home healthcare?
Medicare Eligibility for Home Healthcare Coverage
Individuals must meet specific requirements to be eligible for Medicare home healthcare coverage. First, they must be enrolled in Medicare Part A and/or Part B. Both Medicare Part A and Part B provide home healthcare coverage.
Under Part B, a person is eligible for home health care if she is homebound, requires skilled care, and is certified as needing care by a physician. The added benefit is Part B does not require a qualifying hospital stay.
The essential requirements of eligibility and access to Medicare home healthcare services are: homebound, physician certification, and Medicare-certified agency care.
Homebout, in Medicare terms, means that leaving the home requires a considerable and taxing effort. A physician is the gatekeeper of Medicare home healthcare. The physician certifies and/or recertifies a patient for access to home healthcare. Finally, a Medicare-certified agency must provide home healthcare services, not any healthcare provider.
Medicare Part A Coverage
In contrast, Medicare Part A provides home health care coverage in some situations. A hospital or skilled nursing facility stay triggers Part A. If a person has a three-day inpatient stay at a hospital or has a Medicare-covered Skilled Nursing Facility (SNF) stay, Part A will cover up to 100 days of home health care.
Note that a person must still meet the other eligibility requirements to receive home health care, such as needing skilled care, being homebound, and having a doctor certify that such care is necessary.
A person also must receive home health services within 14 days of being discharged from a hospital or SNF. If a person doesn’t meet all of the requirements for Part A coverage but is otherwise eligible for home health care benefits, her care will be financed under Part B.
Medicare Coverage For Home Healthcare Services Amounts
Regardless of whether Part A or Part B covers a person’s care, Medicare will pay:
- The entire approved cost of all covered home health services.
- Eighty percent of the Medicare-approved amount is for durable medical equipment.
Medicare covers a wide range of home health care visits, including skilled nursing care, physical therapy, occupational therapy, speech-language pathology, and medical social services. These services are typically provided part-time or intermittently, depending on the individual’s needs.
Medicare also covers specific durable medical equipment and supplies, such as wheelchairs, hospital beds, and oxygen equipment.
However, coverage limitations and restrictions may apply, and it’s essential to understand what services are covered and how much you may be responsible for paying out of pocket. The agencies providing the equipment and supplies can give details of costs.
 Limitations and restrictions of Medicare coverage for home health care
Limitations and restrictions of Medicare coverage for home health care
While Medicare provides coverage for many home healthcare services, there are limitations and restrictions to be aware of. For example, Medicare typically only covers part-time or intermittent care and may not cover 24-hour or long-term care.
In addition, Medicare may not cover certain services considered custodial care, such as help with bathing, dressing, and eating. Finally, there may be coverage limitations based on the individual’s medical condition. Some coverage is subject to annual or lifetime caps.
Certified Home Health Agency Disclosure of Covered Costs
Before home health care starts, the certified home health agency must tell the person how much Medicare will pay. The agency must also disclose if Medicare does not cover needed items or services. Then tell how much the person will have to pay for them.
For example, charges to a person may be:
- Medical services and supplies that Original Medicare doesn’t cover, such as prescription drugs or routine foot care
- 20 percent of the approved amount for Medicare-covered durable medical equipment such as wheelchairs, walkers, and oxygen equipment
Tips for Navigating Medicare and Home Healthcare Coverage
Navigating the complexities of Medicare and home healthcare coverage can be challenging, but several tips help make the process easier. First, it’s important to understand your needs and choose the Medicare plan that best fits them.
Second, work with your healthcare provider to ensure that a Medicare-certified agency orders and provides home healthcare services.
Finally, read the fine print and understand any coverage limitations or restrictions that may apply. The Medicare-certified agency is well versed in the cover limitations and costs. Be sure to consult with them ahead of time.
Alternative options for home health care coverage
While Medicare provides coverage for many home health care services, alternative options may be available to better meet your needs. For example, private insurance plans may offer more comprehensive coverage for certain services. Medicaid is another route for low-income individuals.
Private Home Health Care Insurance Policies
Home health care insurance is typically a private insurance policy purchased ahead of time to assist Medicare in caring for someone receiving home health care. The policy covers activities of daily living in the home, such as bathing, feeding, transportation, and housekeeping. Like any insurance, these alternative options must be purchased before the health issues arise. Many insurance carriers offer a variety of these types of policies.
In addition, a variety of community-based programs and organizations offer support and assistance to seniors and individuals with disabilities. These programs may include meal delivery, transportation services, and assistance with daily living activities.
 Home Health Agency Advance Beneficiary Notice of Noncoverage
Home Health Agency Advance Beneficiary Notice of Noncoverage
When a certified home health agency believes that Medicare may not pay for some or all of a person’s home health care, it must give the person a written notice called an Advance Beneficiary Notice of Noncoverage (ABN). The ABN might occur, for example, if the home health agency thinks that Medicare will not pay for items or services because:
- The care is not considered medically reasonable and necessary.
- The care is only unskilled, a home health care aide, like help with bathing or dressing.
- The person is not homebound.
- The person does not need skilled care on an intermittent basis.
The ABN must describe the service and/or items that may not be covered and explain why Medicare probably won’t pay. The notice must also include an estimate of the costs for the items and services so that the beneficiary can decide whether to receive the services, understanding that she may have to pay out-of-pocket for such care.
The ABN also gives directions for getting an official decision from Medicare about payment for home health services and supplies and for filing an appeal if Medicare won’t pay.
How Long Does Medicare Pay for Home Health Care?
There is no limit to the length of time that a person can receive home health care services. Once the initial qualifying criteria are met, Medicare will cover home health care as long as it is medically necessary. However, care is limited. There are a maximum number of visits per week and a certain amount of hours per day of care.
When a person first begins receiving home health care, the plan of care will allow for up to 60 days. At the end of this period, the physician must decide whether to recertify the patient for another 60 days. The patient must be recertified at least every 60 days if home health care is to continue.
Medicare does not limit the number of times a physician may recertify a patient. Provided all eligibility requirements continue, he can recertify an unlimited number.
What Happens When Medicare Stops Paying for Home Health Care?
A home health agency must give a beneficiary a written Home Health Change of Care Notice (HHCCN) when the patient’s plan of care changes because the home health agency decides to reduce or stop providing some or all of the home health services or supplies. Or, the patient’s doctor has changed the orders, which may reduce or stop certain home healthcare services or supplies that Medicare covers.
doctor has changed the orders, which may reduce or stop certain home healthcare services or supplies that Medicare covers.
For example, the doctor changes the care plan from five to three days a week. The agency issues an HHCCN. The beneficiary receives a notification in writing of the change.
The HHCCN lists the services or supplies that will be changed and gives the beneficiary instructions on what to do if she disagrees. The home health agency is not required to give a person an HHCCN when a Notice of Medicare Noncoverage is issued.
Notice of Medicare Noncoverage
When a person’s Medicare-covered services end, the home health agency must give the beneficiary a Notice of Medicare Noncoverage (NOMNC). This notice states when services will end as well as how to appeal the decision. The NOMNC also provides information on contacting the Beneficiary and Family-Centered Care Quality Improvement Organization (BFCC-QIO) to request an expedited appeal.
Once a person decides to appeal and has reached the BFCC-QIO, the home health agency must give the patient a detailed notice explaining why it believes Medicare-covered care should end. The agency should tell the applicable coverage rules and other information about the person’s situation.
A physician must submit a statement of appeal to the BFCC-QIO. It says the patient’s health will be jeopardized if care is discontinued. These factors determine how long Medicare pays for home health care. Knowledge of these rules is vital to maximize benefits and avoid costly mistakes.
Importance of understanding Medicare and home health care coverage
Understanding Medicare and home health care coverage is crucial for seniors and individuals with chronic conditions or disabilities. These programs provide access to essential medical care. They support individuals to maintain their independence and quality of life.
By understanding the different types of Medicare plans, eligibility requirements, coverage limitations, and alternative options, individuals can make informed decisions about their healthcare and ensure they receive the care they need.
Bottomline: Taking Advantage of Medicare and Home Healthcare Benefits
In conclusion, navigating the complexities of Medicare and home healthcare coverage can be challenging, but it’s essential for seniors and individuals with chronic conditions or disabilities. By understanding the different types of Medicare plans, eligibility requirements, coverage

Christopher J. Grimmond
limitations, and alternative options, individuals can make informed decisions about their healthcare and ensure they receive the care they need.
Whether you’re seeking home healthcare services for yourself or a loved one, working with your healthcare provider and understanding the coverage options available is essential. By taking advantage of Medicare and other home healthcare benefits, you can maintain your independence, improve your quality of life, and ensure you receive the care you deserve.
At Omaha Insurance Solutions, we help you understand the many Medicare rules. We navigate you through the forms and get the care you need. Call us at 402-614-3389 to speak with an experienced, licensed insurance agent professional.
 Medicare covers Home Health Care, but the Medicare beneficiary must meet particular criteria, maintain a status of medical need, and follow Medicare regulations and processes to enjoy the benefits.
Medicare covers Home Health Care, but the Medicare beneficiary must meet particular criteria, maintain a status of medical need, and follow Medicare regulations and processes to enjoy the benefits.
Eligibility For Medicare Home Health Care Benefits
- A physician must certify that skilled care is needed and must prescribe the plan of care.
- A participating Medicare-approved home health care organization must provide the care.
- The patient must need at least one of the services: intermittent skilled nursing care, physical therapy, speech-language pathology, and continued occupational therapy.
- The patient must be confined to the home.
Plan of Care
A physician must meet face-to-face with the patient 90 days before the start of home health care or within 30 days after the start of home health care. She must sign and date a certification that the patient needs skilled care and meets all the Medicare eligibility criteria for home health care. As part of the certification, she must determine from the in-person meeting a plan of care.
- A plan of care describes the type of services and care a person will receive for their health concerns. The program will list:
- the variety of services, supplies, and equipment needed.
- the health care professional who will deliver these services
- how often services will be needed
- the beneficiary’s function limitations
- nutritional requirements]
- the results that the physician expects from the treatment
The home health agency is responsible for providing all of the care listed in a person’s plan of care. The agency may do this through its staff or an arrangement with another agency.
The doctor certifies the person as eligible for an initial 60-day benefit period. At the end of the period or before, the doctor may recertify the person, or if the person’s condition has changed, determine the care is no longer needed. Only the doctor can certify the patient or make changes to the plan of care, not the home health agency.
 Medicare-Certified Home Health Care Agency
Medicare-Certified Home Health Care Agency
Medicare will pay for home health care only if a Medicare-certified home health care agency provides it. Medicare approves agencies that meet specific federal health and safety requirements as well as Medicare standards necessary for reimbursement. To ensure that these standards met, Medicare regularly inspects home health agencies. However, Medicare certification does not guarantee a legal warrant of the individuals performing the services.
A Medicare-certified home health agency agrees to:
- be paid by Medicare
- accept only the amount that Medicare approves for its services.
The patient has the right to choose any agency to provide the services as long as they are Medicare certified. The agency is not required to accept the person if it cannot meet that person’s medical needs.
Skilled Care Required But Intermittent
To qualify for Medicare provided home health care, the person needs specialized care. Skilled care means services, such as skilled nursing care, physical therapy, speech therapy, and/or continuing occupational therapy.
The key to determining home health care versus skilled nursing care in a facility is the quantity of care. Home health care must be intermittent. That is, the care must be part-time, meaning less than eight hours each day for up to 21 days–although coverage may be extended in particular circumstances when the need for additional skilled nursing is finite and predictable.
Required Homebound
The homebound criterium does not mean the person is a prisoner in her home. It means leaving is an undue burden. She has trouble leaving home without help because she must use a cane, wheelchair, walker, crutches, or specialized transportation.
It does not mean that person does not leave home on occasion because of important family events, specific medical tests, funerals, or weddings. Even attending adult daycare would not be a violation of being homebound.
Home Health Care May Cover A Health Aide
Home health aide services get a great deal of play. Medicare will cover a health aide for short periods. The aide service must be coupled with home health care  services. Medicare does not cover it exclusively.
services. Medicare does not cover it exclusively.
The home health aide is in support of the healing process with the other skilled nursing professionals. The home health aid does not have a nursing license. For example, a home health aide might help a person with personal care, such as bathing, using the toilet, or dressing–in other words, services that do not require the skills of a licensed nurse.
Other services are help with medications that are self-administered, assistance with activities that are directly supportive of skilled therapy. The aide may help with routine exercises and/or practicing functional communication skills. Where appliable, she may help with regular care of prosthetic and orthotic devices. Medicare will not cover the home health aide if the patient is not receiving skilled care.
Home Health Care Can Cover Social Services
Many injuries and illnesses come with an emotional cost. A patient of my wife recently was hospitalized because his son assaulted him while under the influence of illegal drugs. He was defending his wife, who was likewise being assaulted. The father was hospitalized with broken bones. He is also currently going through chemotherapy treatment and is eighty-six years old.
As you can imagine, the emotional trauma to this couple was extensive and may require counseling and other intervention when the gentleman returns home. Home health care provides these types of services as well.
 Durable Medical Equipment
Durable Medical Equipment
Home health agencies will also help with durable medical equipment. A patient may need a hospital bed, walker, wheelchair, or oxygen. Medicare also covers Medicare supplies, like wound dressings or catheters that are ordered as part of a patient’s care.
If a home health agency doesn’t supply durable medical equipment directly, its staff will typically arrange for a home equipment supplier to bring the items need to the person’s home.
Does Medicare Exclude Some Home Health Care Services?
Medicare does not pay for the following:
- 24-hour-per-day care at home
- meals delivered to the home
- homemaker services like shopping, cleaning, and laundry
- personal care given by home health aides (like bathing, using the toilet, or help in getting dressed)when this is the only care needed.
Does Medicare cover home health care? It certainly does when the patient meets the established criteria. Home health care is a rich source of benefits to beneficiaries that are delivered in a variety of ways and circumstances as needed.
We know what hospitals are. We all have been to a doctor’s office. Many have experienced a relative in a nursing home, but what is home health care?
Home health care is like it sounds. It is the care that takes place in the home. It consists of a wide range of services, like physical therapy, occupational therapy, speech therapy, and nursing care.
The purpose of home health care is short term treatment for an illness or injury, such as a stroke or broken hip. It is about getting the person healthy and independent again. Or, it is for the chronically ill and disabled. The goal is to maintain the highest level of ability and health.
Home health care is not home care. Home care would be services, like housekeeping, bathing, feeding, etc. Medicare does not usually provide those types of personal services, strictly speaking, though there are exceptions at times that allow for a temporary home health aide. It is skilled nursing care provided in the home for those who would not have access otherwise.
Does Medicare Cover It?
Four criteria must be met for Medicare to pay for home health care.
- A physician must certify home health care is necessary.
- The home health care provider must be a Medicare-approved organization.
- The patient must need at least one of the following: skilled nursing care, physical therapy, occupational therapy, or speech therapy.
- The patient must be homebound.
Doctor Certifies Patient For Home Health Care
The doctor must certify a patient needs home health care during an in-person meeting. He signs a certificate certifying that the person meets the Medicare qualification. The doctor lays out a plan of care that care professions implement, and the certification is for 60 days. At the end of the 60 days, or before, he can recertify that patient for an additional 60 days.
The doctor can continue to recertify the patient indefinitely as long as the person qualifies for the medically necessary treatment, and Medicare will continue to cover them.
Home Health Agency Medicare Certified
The home health agency providing the care must be certified by Medicare for the service to be Medicare-covered. In my office building as you come in, a care agency is in the lobby. On the office door, the home health agency lists the various services, and in even bigger letters, it states, “Medicare Certified.”
Medicare certification of a home health agency is an extensive process. Because accreditation is arduous and a source of considerable revenue, home health agencies are very careful about maintaining their certification and advertising their Medicare certification as well. The Omaha metro area has some excellent home health care agencies.
Intermittent Care
Home health care must also be intermittent care. That is, it consists of fewer than seven days a week, or daily care for less than 8 hours each day for up to 21 days. Otherwise, a skilled nursing facility would most likely be recommended for a more intense regimen of care.
Homebound
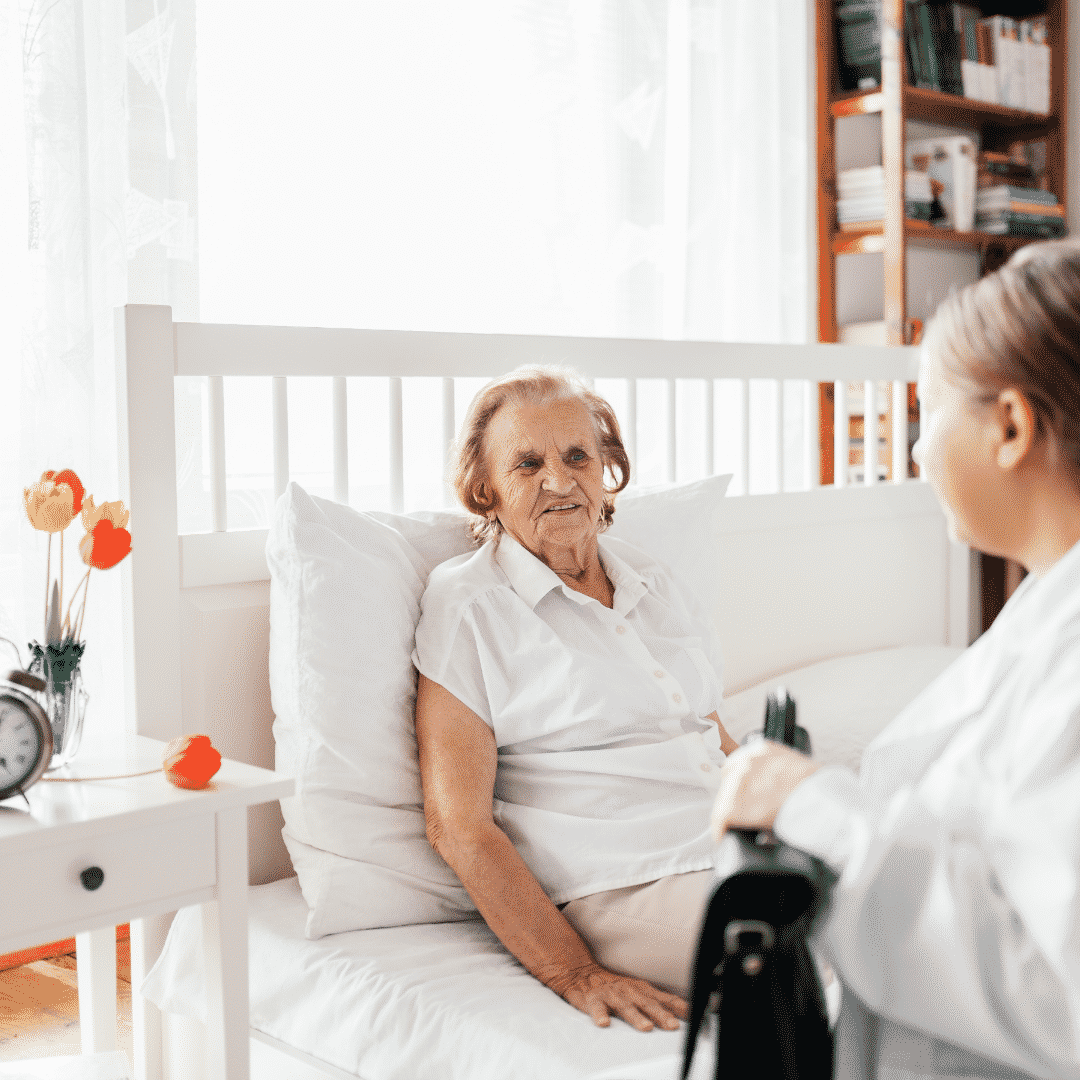 The patient must be homebound, which means she cannot leave her home without great difficulty and requires help, such as a wheelchair, walker, crutches, or specialized transportation. It doesn’t mean she can never leave her home for important things, like family events, hairdressing appointments, some doctors’ appointments, but getting regular health services outside the house would be an undue burden.
The patient must be homebound, which means she cannot leave her home without great difficulty and requires help, such as a wheelchair, walker, crutches, or specialized transportation. It doesn’t mean she can never leave her home for important things, like family events, hairdressing appointments, some doctors’ appointments, but getting regular health services outside the house would be an undue burden.
People are living longer. Tremendous advances in technology have enabled seniors to stay out of expensive skilled nursing care. Nowadays, patients may receive very sophisticated treatment at home and do not need to be institutionalized, keeping the cost of treatment lower. It is an important and essential service that Medicare covers.







